Check your Greatness Profile
The Physician Predicament
A hospital’s success is increasingly dependent on its physicians but physicians have less time and interest in participating in the success of the hospital. Old medical staff structures and medical directorship arrangements are no longer effective in meeting the business development and operational requirements of increasingly focused clinical services. Income pressure and life style expectations have physicians scrambling for new sources of revenue and demanding payment for activities which historically were a voluntary part of medical practice. Collegiality is on the decline as competition between physicians in different specialties increases just when multi-disciplinary chronic care management is catching on. Physicians need innovative business strategies and capital for investments to exploit clinical advances, productivity improvement infrastructure and new business development opportunities but do not plan strategically or retain earnings in their practices.
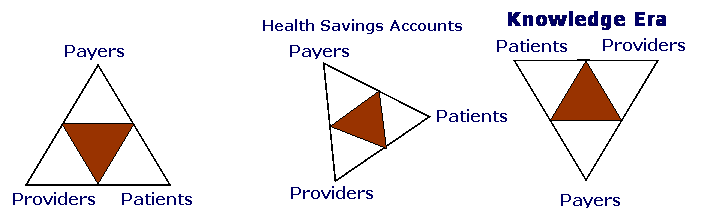
Hospitals and physicians are at risk of being subservient to payers even as consumer driven benefit designs replace managed care certification models. Payers continue to consolidate, building the critical mass of customers to maintain negotiating leverage and investing in infrastructure to maintain a technology advantage. They are also creating golden handcuffs with information and incentives to retain members and providers. Independent organizations and government agencies such as CMS, JCAHO, HealthGrades, U.S. News, and Leapfrog are rating providers on quality and cost. Patients are gaining power through health savings account benefit models that proffer increased choice, higher expectations and incentives to use information to make better decisions. Providers must work together to realign the triangle of power and work with patients in this new era of knowledge to ensure cost effective, quality care.
|
Managed Care Era |
|
Providers |
|
Patients |
|
Payers |
|
Providers |
|
Patients |
|
Payers |
|
Patients |
|
Providers |
|
Payers |
|
Health Savings Accounts |
|
Knowledge Era |
Traditional Physician-Hospital Strategies
Many logical business relationships between physicians and hospitals are thwarted by legal and regulatory constraints. Hospitals have tried several strategic approaches to physician business and organizational relationships, including:
r Paternalism - support all physicians equally so long as they do not threaten the hospital’s core business (speak softly and carry a big stick). This usually entails responding to requests or building consensus around new ideas and often results in only the lowest common denominator projects being implemented. Board participation and/or Joint Board – Medical Staff Committees are the typical ways physicians participate in hospital leadership.
r Magnetism - make the hospital the place key physicians want to practice, focus internally, build loyalty, provide golden handcuffs (if you build it, they will bring their patients). This strategy requires making the hospital convenient and efficient for physicians and often includes remote access to medical records, block scheduling, new medical technology, rapid turnaround times, marketing and advertising and strong nursing support. Paid Medical Directorships and Physician Advisory Committees are employed to expand physician leadership.
r Integration - acquire or manage physician practices, provide recruitment incentives to facilitate growth, joint venture services, proffer financial incentives like gain sharing or paid quality improvement teams (one for all and all for one). Physicians may be included in routine executive meetings or participate on Physician-Administrator service line management teams.
Hospitals have tried a combination of these strategies over the past decade but initiatives are often held hostage by a few physicians who are concerned about being disadvantaged or are satisfied with the status quo or, are simply neutralized by similar actions of competing hospitals. Some physicians are skeptical of a hidden agenda on the part of the hospital or are simply not interested because they are focused on their own practice. Other physicians are moving independently to offer services in their office or their own outpatient (or even inpatient) facility. The hospital leadership may see some strategies as a win-lose proposition or the start of a slide down a slippery slope of erosion of the hospital’s most important sources of profit to support the overall mission of the organization but must understand that if they do not capitalize on opportunities and even cannibalize their own business someone else will. It is often more difficult and more costly to try to erect barriers to competition than to partner with physicians and share the growth. For example, by restructuring in and outpatient nuclear medicine and joint venturing with physicians, lab technician shortages can be reduced, access improved, duplicate capital investment minimized and quality improved. Over the long term, the financial performance of both physicians and the hospital can be enhanced.
Market Realities
As the market continues to evolve, hospitals must move beyond traditional strategies to the next generation of relationships. Just as the introduction of managed care over two decades ago changed the playing field, this new era of knowledge will require a rethinking of strategies. Hospitals and physicians took too long to respond and then often over reacted to the last shift and payers seizes the upper hand, now is the time to reposition for leadership in the management and delivery of healthcare.
CMS has introduced a number of initiatives that require a closer working relationship between physicians and hospitals including:
Ø Medication Therapy Management (2006)
Ø Fee-for-Service Voluntary Chronic Care Improvement (phased in)
Ø Hospital Quality Initiative (clinical and satisfaction reporting and incentive payment)
Ø Hospital Compare (consumer information)
Ø Risk adjusted capitation
Ø Electronic Medical Record and e-prescription adoption incentives
Ø Doctors Office Quality (under development) clinical, practice system and satisfaction measurement and reporting
Ø Health Savings Accounts
Ø Diabetes screening tests
Ø Welcome to Medicare Exam (2005)
There are also new safe harbors for providing physicians with equipment, software and training for electronic prescribing; gain sharing; information linkages and clinical integration.
Payers are already responding with strategies to influence the behavior of physicians and consumers. They have introduced:
Ø Pay for Performance pilots
Ø e-visit reimbursement
Ø Technology support for physicians (e-prescribing, computers)
Ø “Consumer Driven” (high deductible) benefit designs
Ø Web based provider scoring information
Ø Chronic care/disease management programs
Ø Multi-tiered Networks
Ø Expert systems/ decision support tools
Ø Health information/consultation on line
Ø Claims based electronic health record
Never have results (clinical outcomes and cost) been more critical to success. While these factors have gotten lip service for several years, now public perception is changing with the availability of both the tools to measure and report results and incentives to pay attention to them. Success in this environment requires physicians and hospitals to work together for their own enlightened self interest.
The traditional medical staff structure and comprehensive strategic planning process have become obstacles to implementing strategies to capitalize on the new market realities in healthcare. New approaches and new relationships must be developed to meet the varying needs of physicians in different situations and different specialties. These strategies must be highly targeted and cooperatively developed to find common ground and allow unique relationships. Not all clinical services or physician practices are equal in their impact on the success of the hospital nor do they all have the same requirements for success. Hospitals and physicians must work together to create value for themselves and the patients on a service specific level rather than fight over dividing the pie.
Focused business relationships
Hospitals must focus on what they need to be successful and what they can get rather than what they are giving up as they work with physicians to create clinical product lines that can be differentiated and deliver value to patients, payers, physicians and the hospital. This means processes that deliver the best clinical results, cost effective management, high satisfaction, easy accessibility and strong marketing. Not all physicians are going to be willing to work with the hospital on this agenda, even if it is in their best interest. The first and perhaps most difficult challenge will be gaining the cooperation and participation of the physicians. This may require traditional competitors or physicians in different specialties to work together. The benefits must be clear and the process must be simple. The hospital leadership must be willing to take some business risks, share some information and provide some incentives.
1. Define the areas of clinical focus for the hospital. This process must be both quantitative and qualitative. It should involve a detailed clinical, market and financial analysis of narrowly defined clinical product lines and specific services within them. The analysis should consider scope of services, infrastructure, level of care and geographic areas within the market for each service. It should also consider the level of competition, the role, expectations and requirements of physicians involved in providing the service and the decision process of patients. Keep in mind there are several clinical and organizational models that can be utilized and, due to co-morbidities, there is often overlap.
2. Delineate potential benefits for physicians. Benefits are in the eye of the beholder. You must understand the fears and objectives of the physician in order to determine the benefits that might be considered attractive. For some it might be more patients, for others technical revenue or operational influence or access to technology. A strong, data driven case must be developed to recruit physicians to participate in the new relationship. Old beliefs and traditions regarding physicians’ responsibility to the hospital and the practice of medicine must be abandoned and the new reality of the market embraced.
3. Build a business relationship. Results from business relationships between physicians and hospitals have ranged from dramatic increases in market share and vast improvements in clinical and financial performance to the termination and even indictment of CEOs and dissolution of medical groups. Business ventures should be guided by basic parameters that are approved by the board. This might include financial hurdles, mission or strategy fit, operating considerations (e.g. indigent care, billing, restrictive covenants), legal/structural framework and partner requirements/eligibility. These parameters should be specific enough to enable physicians to understand what kinds of relationships are and are not possible yet broad enough to allow the flexibility needed to establish innovative and unique arrangements that meet the specific needs of the market and the partner. Experience suggests that the process must involve physicians sufficiently to ensure that they shape and understand the deal, yet not bog them down in minutia. The simpler and more transparent the arrangement the higher the likelihood of success. Other characteristics of successful business relationships include:
r clearly defined and documented opportunity
r well delineated requirements and contributions (financial, infrastructure, personnel, behavior, outcomes)
r explicit roles, responsibilities, authority and consequences
r careful structuring
r strong leadership
r active monitoring and reporting
r consistent communication
r continual reevaluation
Business relationships with physicians do not exist in a vacuum. Both the unintended consequences and the reaction of others must be considered. There are always some physicians that will be opposed to any business venture. They are often very vocal and sometimes politically and economically powerful. While all objections should be taken seriously, the best interests of the patient and the community should be the primary consideration.
Medical innovations, benefits redesign and regulatory changes are creating new opportunities. New physician business strategies you might consider include:
v Joint new service development plans
v Quality improvement gain sharing
v Service line management/operating ventures
v Geographic coverage payment arrangements
v Quality Institute
v Clinical integration through information sharing
v Chronic Care or Medication Therapy Management venture (CMS fee for service)
v Joint staffing company
v New physician incubator
v E-prescribing, EMR, information or communications Technology
v “Welcome to Medicare” Clinic
v Pay for performance demonstration project
Physicians and hospitals must find ways to work together to improve the quality and reduce the cost of healthcare while protecting their own economic viability. Sound business relationships are critical to accomplishing that.
© CareCompanion 2004